By Sarah Hassing MSN, RN, CCRN
Clinical Educator/Supervisor, Emergency Services, Children’s Emergency Department
WakeMed Health & Hospitals
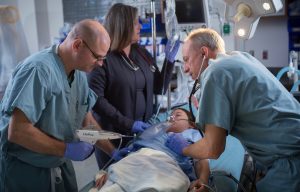
Once upon a time, nurses in the Children’s Emergency Department struggled to administer fluid boluses rapidly to pediatric patients. For over 10 years, we used what we call the ‘push-pull method.’ This consisted of gathering several 60mL syringes, a three-way stop cock, IV tubing, and fluid. Nurses would prime the tubing, connect all the devices and strain to pull and push fluid as fast as they could to crashing patients. Typically, two nurses would trade on and off as their hands would often cramp from the amount of strength needed to effectively push fluid in a timely manner. As difficult as it was, these fluid boluses were essential in the treatment of the pediatric patients as hypotension is a late sign of decompensation in children. The struggle for fluid administration is real!
This struggle changed the day we first started to use the LifeFlow device. Upon the introduction of the LifeFlow, nurses were able to cut down fluid bolus administration times by more than 50 percent. This gave us more time to spend on obtaining vital IV access, administer antibiotics within the ‘Golden Hour’ and turnaround a patient’s clinical presentation almost immediately.
LifeFlow uniquely offers nurses and physicians the ability to rapidly administer fluid without struggling to force a plunger into a syringe. The ease of use of the ‘trigger’ to both prime the tubing and administer the bolus is essential in the rapid administration of fluid. More importantly, utilizing a 10mL syringe makes it easier for a nurse to keep track of how much fluid has been administered with each pull of the trigger instead of adding each varying individual bolus amount that has been drawn up and pushed in. As familiarity with the device increases among providers, staff are becoming more comfortable with its use. In fact, it has become such an accepted use in our hospital, that it is now included in the standard set-up for our pediatric crash carts.
To fully understand the benefits of LifeFlow, you need to see it in action. One example of the impact that LifeFlow made in our emergency department was with a one-year-old infant who came in emergently with fever and respiratory distress. Upon presentation this patient had a temperature of 100F, a heartrate of 210, and a blood pressure of 75/40. The patient’s mother stated he had received vaccinations two days prior and had a low-grade fever but started shaking and turned blue this morning. At first the differential consisted of SVT vs sepsis, so we gave a 10mL/kg fluid bolus to see if it improved the patient’s heartrate. The initial push-pull bolus only dropped the heart rate by 2-3 beats, so the physician assumed the patient had SVT. After two unsuccessful attempts to convert the patient’s rhythm and consultation with the PICU team, it was decided to administer another fluid bolus to the patient using the LifeFlow. In using LifeFlow, we were able to administer 60mL/kg of fluid in less than 5 minutes. With every other pull of the trigger you could watch the patient’s heartrate drop by 5-10 beats. By the time the fluid was in, the patient was calm, his color was improved, and his resting heartrate was 175. Moreover, since it was so easy to set up and administer the fluid bolus using LifeFlow, other nurses were able to obtain IV access and administer antibiotics rather than assist with the fluid administration. It was truly amazing. Since then staff have sung the praises of the LifeFlow to anyone who will listen. In the end it does live up to its name… LIFEFlow is a LIFE-saver!
Note: The information reported here is the opinion of the hospital/author and has not been independently confirmed by 410 Medical. For more reference please see LifeFlow Publications or How it Works for a LifeFlow video tutorial.
Interested in a LifeFlow trial at your hospital? Contact us.