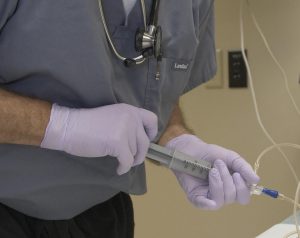
In Part 1 of our blog we presented a 10-year-old girl with suspected septic shock, for whom a fluid bolus was ordered. As recommended by both the PALS and ACCM guidelines, we would push this bolus using a syringe, with either the “push-pull” or “disconnect-reconnect” technique. Both of these are faster than other fluid delivery methods, but they are not without drawbacks.
Have you ever woken up the day after using a syringe for fluid resuscitation to find your hand muscles are sore, or that you have bruise on your palm? Hand fatigue is a major factor affecting the rate of fluid administration when syringes are used. Several studies have evaluated fluid administration with syringes, and in the table below I’ve extrapolated flow rates from these studies to simulate the amount time needed to administer a 60ml/kg bolus using both the syringe methods.1-4
Table 1. Simulated 60 mL/kga fluid bolus using syringe techniques
Patient weight (kg) |
Total fluid (mL) |
Time to complete boluses (minutes) |
Number of syringes or push-pull cycles with 30mL syringe |
|
Disconnect –re-connectb |
Push – pullc |
|||
15kg |
900 |
7.6 – 8.5 |
9.3 – 17.6 |
30 |
20kg |
1200 |
10.2 – 11.3 |
12.4 – 23.5 |
40 |
30kg |
1800 |
15.2 – 17.0 |
18.5 – 35.3 |
60 |
50kg |
3000 |
25.4 – 28.3 |
30.9 – 58.8 |
100 |
a Administered in 20mL/kg bolus sequentially
b Simulated based on 1.77 mL/s delivered1, 1.97mL/s2
c Simulated based on 1.62 mL/s delivered1, 0.85 mL/s4
The table above assumes that providers are able to keep up with a constant rate of fluid administration throughout the resuscitation. Those of us who have used these techniques can attest to how much you slow down after repeatedly pushing the syringe. The larger the patient, the more the syringe strokes, the harder the task becomes. In fact, several of the studies referenced above noted that fatigue increases with the number of syringe strokes.2,4 Interestingly, there was no difference in reported fatigue between push-pull and disconnect-reconnect, even though two people are required for disconnect-reconnect.
Even with smaller fluid volumes, fatigue is a factor. In a study simulating a 250mL bolus (20 mL/kg for a 12.5kg child), 36% of subjects reported some degree of hand fatigue, and complaints of hand fatigue were significantly more pronounced in those who used larger syringes.4
In larger patients, the maximum rate of fluid delivery possible with syringes, combined with fatigue, led to the inability of providers to achieve 60mL/kg in 15 minutes in any patient over 30kg. This makes sense since most of us have experience getting tired and slowing down after 20 strokes! (Stoner 2007)
Using the example of our 10-year-old patient who weighs 30 kg, she could require up to 1800 mL (60 mL/kg) which would take up to 35 minutes based on the flow rates in the studies we reviewed. Even in a 15kg patient, a 60mL/kg bolus within 15 minutes may not be possible using the push-pull method (Table 1).
Although syringes may be faster and have advantages over other fluid administration methods, they may not be fast enough for many patients, as minutes matter in patients with septic shock. Fatigue can have a compounding effect, further decreasing a healthcare provider’s ability to deliver fluid efficiently and reverse shock in critically ill patients.
In the final part of our 3-part series on fluid resuscitation in critically ill children, we will examine the risk of bacterial contamination and user errors that are associated with using syringes for fluid resuscitation.
- Cole ET, Harvey G, Urbanski S, Foster G, Thabane L, Parker MJ. Rapid paediatric fluid resuscitation: a randomised controlled trial comparing the efficiency of two provider-endorsed manual paediatric fluid resuscitation techniques in a simulated setting. BMJ Open. 2014;4:e005028.
- Harvey G, Foster G, Manan A, Thabane L, Parker MJ. Factors affecting pediatric isotonic fluid resuscitation efficiency: a randomized controlled trial evaluating the impact of syringe size. BMC Emerg Med. 2013;13:14.
- Stoner MJ, Goodman DG, Cohen DM, Fernandez SA, Hall MW. Rapid fluid resuscitation in pediatrics: testing the American College of Critical Care Medicine guideline. Ann Emerg Med. 2007;50:601-607.
- Toshniwal G, Ahmed Z, Sengstock D. Simulated fluid resuscitation for toddlers and young children: effect of syringe size and hand fatigue. Paediatr Anaesth. 2015;25:288-293.